T: 01822 851370 E: [email protected]
Visit RSN Survey about life in rural England to find out more.
November Edition of Casebook from the Rural Health and Care Alliance

November 2020 Edition
In Casebook this month: a bevy of stories about the coronavirus and its multifaceted impact on many aspects (if not all aspects!) of our lives. I also reveal some really interesting happenings in connection with the development of the work programme of the National Centre for Rural Health and Care, particularly in the context of the launch of our Rural Proofing Toolkit for Health and Care on 9 December – be sure to book your space, full details below.
NEWS COMMENTARY
Give health workers indefinite right to remain in the UK, urge cross-party MPs
Workforce is a crucial issue in rural England in terms of health and care – this is a powerful story in this context.
A cross-party group of MPs is calling on the government to make provisions for everyone working in the NHS or social care during the pandemic to be given the automatic right to stay in the UK.
MPs from Labour, the Liberal Democrats, the SNP, Green Party, Plaid Cymru, the DUP, SDLP and Alliance have written to Jacob Rees-Mogg, the Leader of the House with responsibility for the government’s parliamentary timetable, urging him to grant time to debate and pass a bill giving health and social care workers indefinite leave to remain in the UK.
Earlier this year, health workers were offered a free extension of their visas if it was due to expire before October 2020. Those whose visas expire after that date “are already being forced to choose between paying to renew their visas or leaving the country”, the MPs write.
The bill, presented by Christine Jardine from the Liberal Democrats with cross-party support, was due to be debated in parliament earlier this month, but has been postponed until next year due to a government move to push back all private member’s bills. These MPs are calling on the government to allow time for the bill to be debated and passed in government time, as soon as possible.
Christine Jardine, the Liberal Democrat MP who has proposed the bill with cross-party support, said: "So many of the people who have kept the NHS going through this crisis are now at risk of losing their jobs thanks to the Home Office's heartless refusal to extend their right to work here in the UK. The last thing we need right now is to lose yet more valuable NHS and care staff, but this is what we will see if the Home Office do not change course.
Full article:
https://www.newstatesman.com/politics/staggers/2020/11/give-health-workers-indefinite-right-remain-uk-urge-cross-party-mps
Coronavirus: Inside test-and-trace - how the 'world beater' went wrong
In such a rich country we are surprisingly bereft of heft and nous in the context of the test and trace agenda. This article provides a few clues as to why this is the case. It tells us:
Just half of close contacts given to England's NHS Test and Trace are being reached in some areas, a BBC investigation has found.
Six months after Boris Johnson promised a "world beating" system, it can be shown the network is failing in areas with some of the worst infection rates.
The research also found no-one from NHS labs was at a key government meeting with private firms about testing.
But the government said the system was "undoubtedly" curbing Covid spreading.
It added that NHS Test and Trace was dealing with rising numbers of cases and was working hard to "refine and improve" the way it worked.
The companies and their leaders involved with testing had "hundreds of years" of experience in the field, it said.
As ministers struggle to get test-and-trace on track, BBC News spoke to key government figures, scientists and health officials who were involved from the very start to establish what went wrong - and, crucially, whether the system can be fixed to hold the virus in check until vaccines come to the rescue. The investigation found a system performing worst in the areas where it is needed the most and still struggling with the legacy of decisions that were made at the outset.
Further revelations include the fact that a move to more local contact tracing by councils was being undermined by IT problems, leading to a reliance on spreadsheets and delays getting contact details.
Full article:
https://www.bbc.com/news/health-55008133
Poor areas of England face 'permanent' lockdown, says public health chief
Let's not forget some of the areas pertinent to the theme in this article are rural. It tells us:
Some of England’s poorest areas face being trapped in coronavirus restrictions “permanently” unless the government tackles deep-rooted inequalities that are driving high transmission, according to a public health chief.
Prof Dominic Harrison, the director of public health at Blackburn with Darwen council, said the government’s “pointlessly punishing” approach would keep areas such as his under strict measures up to next summer.
He told the Guardian: “We do need the restrictions, but what we need is something that is going to be more effective, more helpful, less pointlessly punishing than continued controls that aren’t going to be effective, or that are unlikely to be effective in the medium term and cause continued and further economic damage.”
Boris Johnson is expected to announce the planned route out of England’s national lockdown next week. The lockdown is due to end on 2 December. Areas with the highest infection rates are expected to remain in the highest tier of restrictions, meaning the continued closure of non-essential retail, pubs and restaurants.
Blackburn has had more coronavirus cases relative to its population than any other part of the UK, despite having been under various forms of local restrictions since July. The Lancashire town has recorded 5,833 cases per 100,000 people since March. The next highest rates are in Oldham (5,667), Manchester (5,205) and Rochdale (5,078).
Full article:
https://www.theguardian.com/world/2020/nov/18/poor-areas-of-england-face-permanent-lockdown-says-blackburn-public-health-chief
Covid: Oxford vaccine shows 'encouraging' immune response in older adults
Bearing in mind the skewed demography of rural England this is very good news. The story tells us:
The Oxford coronavirus vaccine shows a strong immune response in adults in their 60s and 70s, raising hopes that it can protect age groups most at risk from the virus.
Researchers say the Lancet phase two findings, based on 560 healthy adult volunteers, are "encouraging".
They are also testing whether the vaccine stops people developing Covid-19 in larger, phase three trials.
Early results from this crucial stage are expected in the coming weeks.
Three vaccines - Pfizer-BioNTech, Sputnik and Moderna - have already reported good preliminary data from phase three trials, with one suggesting 94% of over-65s could be protected from Covid-19.
The Oxford data is from an earlier stage, which tests the safety of the vaccine and the body's response to it, but in the long run it's likely this vaccine could be easier to roll out because it doesn't need to be stored at very cold temperatures.
The UK government has ordered more of the Oxford vaccine, manufactured by AstraZeneca, than any other - 100 million doses - compared to 40 million doses of the Pfizer-BioNTech vaccine and five million of the Moderna vaccine.
Full article:
https://www.bbc.com/news/health-54993652
Report calls for ‘digital health hubs’ to tackle health inequalities in England
We know the people in Nailsea featured in this article. More of their dynamism would enable us all to get to grips with this issue. This story tells us:
An NHS-commissioned report into digital inclusion in health and care calls for ‘digital health hubs’ to prevent exclusion from further widening health inequalities.
The charity, Good Things Foundation, carried out the review into the NHS Widening Digital Participation programme, which took place between 2017 and 2020, in partnership with NHSX, NHS Digital and NHS England
According to the report, digital inclusion should be embedded in local health and wellbeing strategies, with the public involved in co-designing digital health services. This should include solutions for those who have low digital skills and face barriers to health care.
Digital health hubs aim to use community engagement to reach poorly-served groups and support access to digitally-enabled health care and wider wellbeing. They could be based in libraries, GP surgeries or other community spaces.
A prototype created in Nailsea, Somerset, was run by volunteers and helped people build digital confidence, signposted to local health activities, and motivated healthy behaviour change.
The report says that digital access has become a social determinant of health. Being able to afford internet access and having access to digital skills to use the internet safely are now essential to wider determinants of health.
Full article:
https://www.healthcareitnews.com/news/emea/report-calls-digital-health-hubs-tackle-health-inequalities-england
NATIONAL CENTRE UPDATE
Parliamentary Inquiry
Great Parliamentary Inquiry Session - covering the whole globe, with speakers from New Zealand to the USA earlier this month. Members can learn more and come along to the final session we have planned in December if you email us.
Rural Proofing Health Toolkit Launch – Book Your Space
This is being launched on 9 December – it has its origins in some really insightful work by Brian Wilson of Rural England and Billy Palmer of Nuffield Trust. There are great opportunities for members to access it and a package of support to implement it. Click here to book your place at the launch.
Covid Dashboard
This initiative, which is a joint endeavour between the National Centre and Nuffield Trust will be launched soon. It will help you understand the broader impact of the pandemic on health inequalities and outcomes in your area.
Membership Review
We have been reviewing the benefits linked to our joint membership scheme. We would love to know more about your thoughts in that regard. You can email us to let us know if there is anything you would like as an RHCA member. Covering all aspects of membership, we now have approaching 200 organisations in membership.
Research
The partnership between the National Centre and the Institute of Rural Health at the University of Lincoln is gathering pace. We have committed to work together to look at the impact of the English Indices of Deprivation on health and care policy, to review the key workforce challenges which the centre is aware of and to progress our joint input into the national pilot Centre for Future Living on the Lincolnshire Coast in Mablethorpe.
Members Research Interests Survey
A big thank you to the member organisations that have taken part in our Members’ Interests Survey. The survey is still live so if you haven’t yet completed it click here.
The results from this so far show that the three most common areas of interest are: accessibility of services, long term health conditions and remote and digital health services.
There is a large overlap of research interests in many other areas, including mental health, the cost of rural healthcare, digital infrastructure, evaluating social impact, and in supporting older service users. The results are shown in the graph below, and have also been formatted into a matrix table so that members can find out which other members share their interests. The NCRHC is always very happy link up members where there may be opportunities for collaboration or shared learning, so please get in touch if you would like us to facilitate an introduction. The NCRHC’s intention going forward is to pilot the use of online forums where members with related interests can network and share information. We hope to have the first of these forums up and running by December, so please look out for emails inviting you to join.
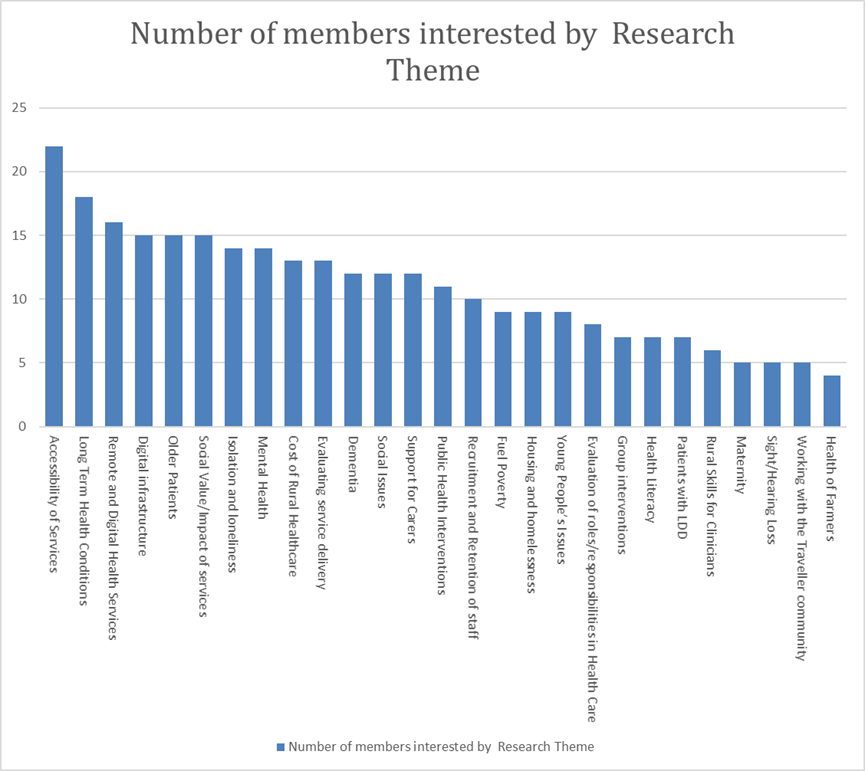 |
To see a further breakdown of this table and the names of organisations interested in each research area click here
Opportunities for Research Collaboration
A number of member organisations have indicated that they would be keen to collaborate on research projects. Including LIVES, Community Heartbeat Trust, Lincolnshire Refugee Project and Somerset NHS Foundation Trust.
LIVES
Are looking for an academic partner to write an evaluation paper on the CEMS model of delivery- one on evaluation on service delivery and outcomes, and another could be written from a workforce angle. Funding is needed.
Community HeartBeat Trust
Are looking for an academic partner to undertake some research into the public’s attitudes towards community defibrillation
Lincolnshire Refugee Doctors Project CIC
Are looking for a partner to support them to evaluate the effectiveness of their programme of supporting refugee clinicians into roles within the NHS.
Somerset Partnership NHS Foundation Trust
Are looking to evaluate the outcomes the COVID-19 pandemic had had on their Trust.
If you can help, and would like us to facilitate an introduction please contact [email protected]
FUNDING OPPORTUNITIES
This month we focus on two funds namely: the Gamesys Foundation with funding for mental health; and the Garfield Weston Foundation with funding available to a wider range of sectors including health. To find out more about each of these funds click here
Gamesys Foundation
The main focus of the Gamesys Foundation is to “preserve and protect the wellbeing of individuals suffering from mental health issues”.
They provide grants and funding to charitable organisations (charities, CICs, CIOs) who care for individuals directly, as well as those who focus on research in the mental health field. The income of the organisation applying must be greater than £50,000 per annum, and applications can be made at any time of the year.
Garfield Weston Foundation
The Foundation supports a broad range of charities across the UK that make a positive difference. We fund a wide range of causes and charities and our grants vary according to the size of the charity and the work being undertaken. Areas supported include Arts, Community, Faith, Health, Education, Environment, Youth and Welfare. They offer two types of grants; Regular Grants For applications below £100,000. These applications are reviewed by our Trustees on an ongoing basis so there are no specific deadlines. Major Grants for applications of £100,000 or more are reviewed at one of the Foundation’s eight Board meetings a year.
MEMBER SHOWCASE
 “Our Priority Services Register (PSR) is there to help our customers when and where they need it the most.
“Our Priority Services Register (PSR) is there to help our customers when and where they need it the most.
As well as offering a wide range of options such as large print or braille bills, we also make sure customers who are signed up will be supported in the event of an interruption to their water supply.
Registering yourself or helping your family, friends and neighbours to register gives you extra reassurance in these uncertain times.
Our particular focus for the PSR over the next five years, is:
- Increasing the number of ways our customers can reach us in an emergency
- Advising customers on how to save water and money
- Helping residents protect their homes against costly leaks and bursts.
If you are a South East Water customer and would like to register for Priority Services, please fill in our secure online form at www.southeastwater.co.uk/priority or call our dedicated Customer Care Team on 0800 952 4000. We're here Monday to Friday between 8am - 7pm, and Saturdays between 8am and 1pm.
Even if you don't need these services yourself, you may have a family member, friend or neighbour who might benefit from a little extra support, so please let them know about Priority Services. It's completely free to our customers and you don't have to be the named bill payer to benefit from them.”
We’d love to hear from you - share what you’re proud of
The RHCA provides news, information, innovation, and best practice. If you have something, you would like us to feature in a future edition, please let us know by clicking here to send us an email.
Spread the word
If you know of other organisations that you think would benefit from joining the Rural Health & Care Alliance, please click here to email us and let us know.
RURAL SERVICES NETWORK
Up to date news on Health and Care
The Rural Services Network provides a useful source of themed news content and data. Check out the latest news on Health & Wellbeing and Vulnerability, where you’ll find articles on a diverse range of rural issues affecting rural communities . You might also find this research on Over 65 Population Projections useful too.
| The Rural Health & Care Alliance is a membership organisation administered by the Rural Services Network on behalf of the National Centre for Rural Health & Care. Explore the RHCA service below: |
 |
 |
 |
 |
 |
 |
 |
 |
 |
 |